Request an Appointment
(703) 719-2040

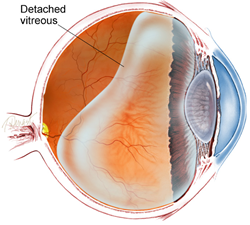
Inside the middle part of the eye, between the lens and the retina, is a large section known as the vitreous chamber. This chamber contains a clear fluid called the vitreous. Although the vitreous, a gelatinous liquid, initially has a firm jelly-like consistency, it can liquefy, shrink and separate from the retina as a part of the aging process. When this happens, a few clumps of the vitreous may break away from the edges and start to float in the more liquid center. With entering light, these floating strands cast a shadow on the retina that create the appearance of drifting spots or threads.
Over the course of 1 to 3 months, the vitreous gel further condenses and the sides of the gel also separate from the retina until the PVD is complete and the vitreous gel is attached to the retina only at the vitreous base
These symptoms usually become less intense over several weeks or months. Most patients experience PVD after age 60, once in each eye, and the condition is usually non-sight-threatening but occasionally affects vision more permanently in the event of a complication, such as retinal detachment or epiretinal membrane.
Mild floaters in the vision are normal, but a sudden increase in floaters is often the first symptom of PVD.
During PVD, floaters are often accompanied by flashes, which are most noticeable in dark surroundings. Most patients experience floaters and flashes during the first few weeks of a PVD, but in some cases the symptoms are hardly noticeable. If PVD is complicated by vitreous hemorrhage, retinal detachment, epiretinal membrane, or macular hole, the flashes and floaters may be accompanied by decreased or distorted vision.
\While floaters in the shape of thread-like strands, dust, cobwebs, a circle, or small shadowy dots can get annoying, they are most bothersome when near the center of vision and less annoying when they settle to the side of the vision. However, in some cases, floaters and flashers indicate a more severe condition that can lead to vision loss.
According to statistics, about 70% of the population experiences a floater at some point in their lives. While you may not notice your floaters throughout the day, at various times, they may appear to drift aimlessly in front of your eye. They can be particularly annoying and noticeable when you are gazing at a blue or overcast sky or a computer screen with a white or light-colored background. Floaters appear to move as your eyes move and then dart away when you try to look at them directly.
Posterior vitreous detachment is rare in people under the age of 40, and increasingly common during advanced age.
Additional risk factors for PVD include myopia (nearsighted- ness), trauma, and recent eye surgery such as a cataract operation. Patients who experience PVD in one eye will often experience PVD in the other eye within 1 year.
If a PVD progresses gently, gradually, and uniformly, the symptoms are typically mild. PVD is non-sight-threatening and the symptoms subside in the vast majority of patients. Most patients no longer notice flashes after months and floaters tend to improve. No specific treatment is needed for PVD.
However, if the forces of separation are strong or concentrated in a particular part of the retina, or if there is an abnormal adhesion between the vitreous gel and the retina (such as lattice degeneration), the PVD can tear the retina or a retinal blood vessel. Flashes and floaters are typically more obvious when PVD is complicated by a retinal tear or vitreous hemorrhage. These conditions can lead to further complications, such as retinal detachment or epiretinal membrane, which can result in permanent vision loss. Complications of PVD are rare but can be serious and require urgent treatment, such as laser for a retinal tear or surgery for a retinal detachment. For this reason, one or more checkups are recommended within 3 months after the onset of PVD.
If you experience a sudden onset or abundance of floaters and spots, flashes of light in the same eye as your floaters, or notice peripheral vision loss, it's essential to get immediate care.
